 Several studies show that DREZ lesioning produces excellent pain relief in the early postoperative period with 75% to 98.2% of patients having good results immediately after surgery. If pain persists despite medical management or surgical repair, other invasive treatment modalities like DREZ lesioning and cervical SCS are indicated.įor many, DREZ lesioning is the preferred procedure for treating intractable pain due to brachial plexus avulsion. Surgical procedures for repair of brachial plexus lesions, like repair with autologous grafts, extraplexual or intraplexual nerve transfers, are reported to help in relieving the pain in some cases. Patients are initially treated medically with a combination of anticonvulsants, antidepressants, nonsteroidal anti-inflammatory drugs, or opioids. This pain is unfortunately very resistant to many forms of therapy. It is thought that the lack of sensory input into the spinal cord leads to spontaneous activity of the neurons in the dorsal horn, thereby causing pain. The origin of the pain has been attributed to root avulsion and spinal cord deafferentation. The pain usually begins within days of injury and generally persists. In addition to the constant pain, patients typically complain of periodic sharp paroxysms of pain lasting several seconds. Most patients describe the pain as a burning sensation, or similar to pins and needles, or an electric shock. One of the most serious and disabling consequences of brachial plexus avulsion is chronic pain with an incidence of 80%. Most brachial plexus avulsion injuries are traumatic in origin, mainly caused by motor vehicle accidents or industrial injuries. Permanent paddle cervical spinal cord stimulation. On 1-month follow-up, the patient continued to report a good coverage of his pain with no recurrence. 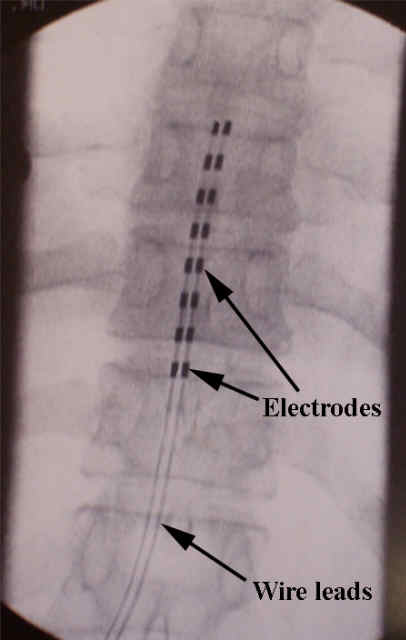
An SCS with paddle-type leads was placed by a neurosurgeon covering the area from C3 to C5 (Figure 0002). Decision was made to proceed with implantation of a permanent stimulator. On his follow-up visit, the patient reported a 50% reduction in pain intensity and was satisfied with the result. We fixed the stimulator in place and asked the patient to monitor the efficacy of the stimulator on decreasing his pain level and improving his quality of life and to return to the clinic in 3 days. With stimulation the patient reported a decrease in his pain level with complete coverage of his right upper extremity and right shoulder. The electrodes were covering the area from C3 to C6 (Figure 0001). Under fluoroscopy guidance, we advanced the lead until the tip was seen at the C3 level. We entered the epidural space at C7-T1 level using a paramedian approach. Decision was made to proceed with a cervical spinal cord stimulator trial. Medical management with a combination of an antidepressant, an anticonvulsant, a nonsteroidal anti-inflammatory medication, and an opioid failed to improve his pain. He was not interested in functional recovery and was only concerned about relieving the pain. On examination, he had no sensation or motor function below the deltoid. He described his pain as burning, stabbing, and sometime like an electric shock, starting at the shoulder and radiating to the arm and his five fingers, with an intensity of 7/10 on a numeric pain rating scale. He lost sensation and motor function below the deltoid in his right upper extremity, however his main debilitating problem was severe chronic pain. 
Magnetic resonance imaging (MRI) showed complete nerve root avulsion from C6 to T1. He suffered from multiple injuries including injury to his right brachial plexus. We report a case of significant improvement in pain from brachial plexus avulsion injury after implanting a cervical SCS.Ī 25-year-old male patient was involved in a motor vehicle accident 5 years ago. Cervical spinal cord stimulation (SCS) is one of the underutilized treatment modalities with several reports of good outcome. However, in most cases, the pain is resistant to medical treatment and has a high-recurrence rate after invasive procedures like dorsal root entry zone (DREZ) lesioning. The pain can be treated medically or with more invasive surgical procedures. Almost 80% of patients with brachial plexus avulsion develop chronic pain. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
